Acute and subacute pain
Pain is triggered when there is tissue damage (tendon, muscle, bone, etc.) following an injury, accident, or illness. It results from interactions between multiple neurons (nerve cells) and danger receptors known as nociceptors.
The International Association for the Study of Pain defines pain as “an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage” (IASP).
When an injury occurs, acute pain serves as a reminder to temporarily protect the injured area.
Tissue healing generally occurs within 4 to 6 weeks following an injury. During this process, damaged fibres rebuild according to their function. Pain evolves along this healing cycle and becomes subacute. However, prolonged immobilization can lead to tissue stiffness, which can itself become a source of pain. It is therefore important to gradually resume activities during the healing phase.
With proper injury management and adequate recovery, pain normally subsides once the body has completed healing.
What about persistent pain?
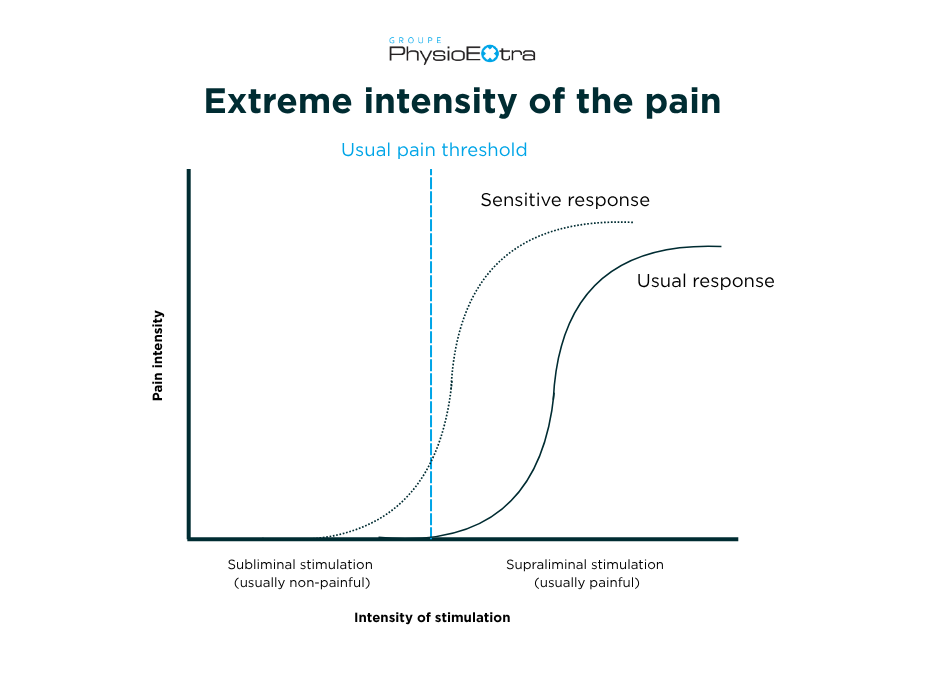
Sometimes, after an injury, physiological changes occur within the nervous system, causing it to remain in an alert state. The circuits that transmit pain signals to the brain become more sensitive, a phenomenon known as peripheral or central sensitization.
The alarm system then activates at a much lower threshold than before. For example, pressure that would normally be harmless may be perceived as painful. Pain, initially useful for protecting the body, becomes a false alarm maintained by various factors.
Even once tissue healing is complete, the body may continue to react as though there is danger, maintaining muscle contractions, tension, and protective behaviours.
Over time, pain may intensify and lead to persistent disability.
The brain itself can also become sensitized to pain, a process known as central sensitization. Many factors can influence the persistence and intensity of pain, including stress, depression, sleep quality, lifestyle habits, and nutrition.
Pain is considered chronic when it remains present beyond the normal healing period or persists for more than three months (Government of Québec).
Chronic pain then becomes a condition distinct from the initial injury.
Risk factors for sensitization
Three main categories of factors contribute to the development of hypersensitivity:
- Biological factors: poor physical conditioning, poor posture, sedentary behaviour, prolonged immobilization, unhealthy diet, lack of sleep, tobacco or alcohol use.
- Psychological factors: stress, anxiety, depression, catastrophizing, low self-esteem, and lack of social support.
- Organizational factors: stressful work environment, conflicts, job dissatisfaction, or difficult relationships with colleagues.
Preventing sensitization
Conversely, certain elements can help prevent the onset or worsening of persistent pain:
- Adopting good posture and proper ergonomics
- Engaging in regular, appropriate physical activity
- Maintaining good sleep hygiene and effective stress management
- Eating a balanced diet
How can persistent pain be treated?
Persistent pain can significantly limit function and affect mood as well as participation in meaningful activities. However, it is not inevitable.
Self-management involves using various strategies to cope with chronic pain and reduce its impact (Douleur Québec).
Recommended strategies
- Consult a healthcare professional to better understand persistent pain and the factors influencing it. Improved understanding is associated with reduced emotional distress. An educational video is available here: Understanding persistent pain.
- Engage in safe and appropriate physical activity to reduce fear of movement and improve physical capacity. Physiotherapists, occupational therapists, and kinesiologists can support this process.
- Explore yoga, when taught by a qualified instructor, to improve overall mobility and body awareness.
- Use meditation and relaxation techniques to better manage pain.
- Participate in a multidisciplinary functional restoration program involving physiotherapists, occupational therapists, kinesiologists, and sometimes psychologists (Douleur Québec).
- Use appropriate medication when recommended by a physician.
- Work on stress management, social support, and internal dialogue, with the help of mental health professionals when appropriate.
Support services are also available for people living with persistent pain:
In summary
- Acute pain is a useful alarm, while persistent pain is a false alarm linked to nervous system sensitization.
- A gradual return to activity after an injury is essential to prevent chronic pain.
- Biological, psychological, and environmental factors influence pain persistence.
- An interdisciplinary approach, including physiotherapy and kinesiology, supports better management of persistent pain.
- Mental health professionals play a key role in addressing the psycho-emotional aspects of pain.
Living with persistent pain? Appropriate care can help you better understand your pain and regain an active lifestyle. Consult a professional to begin a personalized approach.
Other sources
- Jam B. The Truth About Pain. Advanced Physical Therapy Education Institute, Thornhill, Canada, 2010
- Butler D & Moseley L. Explain Pain. NOI Group Publications, Adelaide, Australia, 2003
- Bigos S, Roland M, Waddell G, Klaber J, Burton K, Main C. The Back Book. TSO Information & Publishing Solutions, Norwich, United Kingdom, 2002
- Woolf CJ. Central sensitization: Implications for the diagnosis and treatment of pain. PAIN (2010), doi:10.1016/j.pain.2010.09.030
- Moseley L. Understanding chronic pain. Physical Therapy Reviews 2007; 12: 169–178






